Smart, smarter, smartest… the Philips route to superlative healthcare solutions
In conversation with Casper Garos, Frank van der Linden and Herman Stegehuis
Recent decades have witnessed phenomenal advances in healthcare. But the combination of longevity, chronic disease and costs have made the need for smart solutions paramount. The growing presence of healthcare in the RD&I landscape has been making its mark within the ITEA Community, so time to reflect on the input and impact of Philips over the past seven or so years. This brief retrospective of Philips' very active involvement in the (smart) healthcare projects within the ITEA Community bears testimony to the key role it has played and continues to play, one that benefits business, users, knowledge and, most important of all, patients.
"As global leader in medical diagnostic imaging and patient monitoring, Philips' healthcare innovation revolves around improving the quality and efficiency of healthcare through a focus on continuum of care, central to which is a patient-centric approach. In combining its expertise in medical technology with the clinical know-how of its customers to produce innovative solutions, the focus lies on two main domains: imaging and IT architecture. Herman Stegehuis explains: "All kinds of imaging techniques are applied to provide support during diagnostics and therapy while IT architecture is geared towards the communication aspects, such as gathering and integrating data so that the information can be used efficiently and effectively. These two domains, which often overlap and interconnect, enable patients to be treated - through minimally invasive surgery or tele-medicine, for instance - that would not otherwise be able to be treated, shorten hospitalisation and rehabilitation time for patients, make procedures and processes more efficient and reduce the escalating costs of healthcare." Both domains are evident in the ITEA projects that Philips has led in recent years.
Maximum impact, minimal invasion
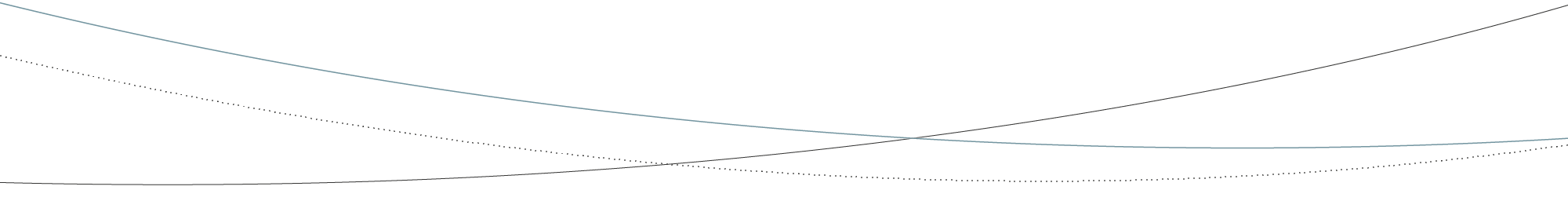
Going back five years or so, to the completed ITEA 2 EDAFMIS project, Frank van der Linden reveals how important a role information technology could play in the modern operating theatre, especially to meet the growing demand for minimally invasive surgery. "The problem was that surgical operations were not well supported by IT; too many independent systems were trying to communicate with each other. On top of that, surgeons did not have access to modern IT solutions such as decision-support systems." EDAFMIS brought together a group of healthcare equipment companies in the Netherlands with a major computer software company in Turkey to change this and develop a new generation of medical operation support systems. The result was a software package for imaging and intervention that enabled easy interoperability and user interaction, providing a minimal operation cockpit that supports automation and navigation, and ultimately a marked improvement in quality and speed of treatment in operating theatres.
"I think when we did the first procedure with EP navigator here it was like a new dimension, because there was so much new information… 3D information adds a certain level of confidence when you do mapping and ablation procedures."
Dr. M. V. Orlov, St Elizabeth's Medical Center, Boston, USA
On EP-cockpit (EDAFMIS)
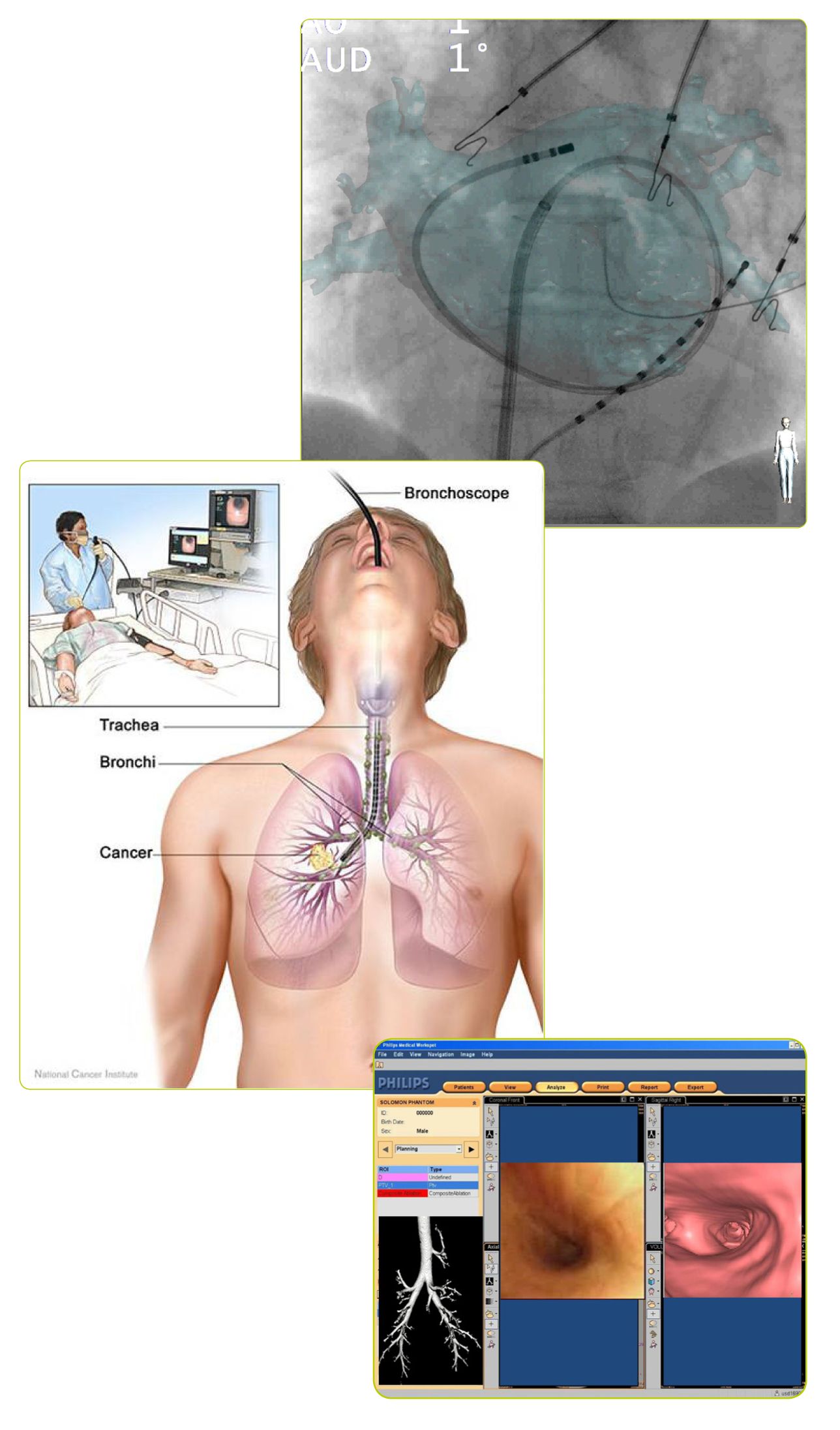
High-performance computing reduces healthcare costs
Finishing at more or less the same time as the EDAFMIS project, and also coordinated by Van der Linden, the HiPiP project aimed at developing affordable high-tech medical image-processing applications based on high performance computing multicore, multiprocessor technologies. "Real-time image processing has become increasingly important in healthcare," Van der Linden stresses, "particularly for minimally-invasive operations, automated screening and medical research." With massive amounts of data to be processed, the key was to use parallel processing technologies to make faster use of this information - ideally in real time - especially for applications of faster 2-, 3- and 4-D - space and time - images like detailed brain imaging, minimally invasive surgery, real-time radiation therapy planning, mass screening for early cancer detection and faster operation of highresolution transmission electron microscopes. HiPiP has not only increased speeds but also improved real-time aspects of multicore processing - particularly the predictability of images being shown in a very short time with little variation in the time taken to process the images. This now enables a doctor to see an image taken a tenth of a second earlier, allowing much improved hand-eye co-ordination when using advanced image processing during surgery. The significant progress achieved in the ITEA 2 project enabled four of the partners to launch a series of different products on the market in 2012 based on HiPiP results. Furthermore, the project has boosted Europe's position on the global stage with a greater understanding of real-time parallel processing.
Healthcare dilemmas in an ageing population
Rising healthcare costs and shortage of personnel present real challenges and healthcare innovation is being pushed to the limit to come up with suitable clinical and technological solutions. Care4Me (project leader Frenk Sloff) set out to improve quality and productivity in healthcare using advanced medical imaging and decision-support methods with the ultimate goal of developing clinical prototypes for early diagnosis of cancer, cardiovascular and neurodegenerative diseases connected to hospital information systems in a new systems architecture. The consortium involved large and small medical equipment manufacturers, research institutes and academic hospitals and its main outcome can be summarised as an open and dynamic hospital-wide, service-oriented architecture that integrates models of anatomy and pathology, computer-aided detection and diagnosis components as well as decisionsupport tools. Care4Me helped to strengthen the competitive position of Europe, especially its consortium partners, and the exploitation potential for cardiology tools and products and fast exploitation of the results was evident in a number of software packages, including QCA-3d by Pie Medical, Qivius by Medis and ClarityIQ by Philips Healthcare. Ultimately, of course, it is the patient that benefits - through better care and lower healthcare costs.
"This dose reduction is, at least in my mind, a real quantum leap in reducing the dose and improving thereby the procedure both for the patient and for us. I think it's really fantastic."
Dr. T. Andersson, Interventional Neuroradiologist, Karolinska University Hospital, Stockholm, Sweden
On Clarity-IQ (Care4Me)
Boosting health on three fronts
With global healthcare spending at around 15% of world GDP in 2015, the drive to increase hospital efficiency and reduce the average length of stay for acute care cannot be overstated. Herman Stegehuis, the MEDIATE project leader, explains that "the focus was on cardiology, oncology and orthopaedics in developing system architectures to enable the integration of multi-modal systems, support multi-vendor interoperability, allow integration of third-party solutions and facilitate user interaction. The resulting set of technologies improves not only healthcare practitioners" knowledge of the condition of individual patients but also the predictability of procedures, reducing complications and obtaining better clinical outcomes from treatment." Key MEDIATE consortium member, Barco, used the results of the MEDIATE project to create its Nexxis platform, an IP-centric solution for video and image management and distribution in the next-generation digital operating room and over 500 operating rooms within Europe have installed Nexxis. In commercial terms, the diagnostic and interventional medical imaging market is substantial, worth almost €20 billion globally, and growing steadily at an average compound annual growth rate (CAGR) of about 4%. "The future healthcare challenges being faced by society create, of course, opportunities for the kinds of innovations being generated in projects like MEDIATE," Stegehuis adds, "and they are not restricted only to the healthcare imaging market. Some of the techniques that have been developed in MEDIATE can be used in other domains like traffic and microscopy." In addressing a major societal challenge, MEDIATE delivered a very powerful impact on both revenue and jobs, and brought together a large number of innovations.
MEDUSA: three new healthcare concepts
The recently completed MEDUSA project, with Frank van der Linden at the helm, enhances the quality of diagnosis and decision-making in acute and/or critical situations in a patient's condition by introducing the integrated combination of three new, healthcare service concepts - advanced imaging, secure virtual workspaces and medical diagnosis support. It paves the way for new, commercial services in the European healthcare business by offering a combination of advanced real-time image processing, real-time decision support, secure and rapid exchange of massive data sets within virtual collaborative workspaces. MEDUSA provides solutions to on-demand, high-performance image processing, all of which share the common cloud-based framework. The collaboration and results have spawned a number of spin-offs, including NICo-Lab, created to leverage market access for the MEDUSA cutting-edge research results. Philips' own strategy aims to provide an infrastructure as service (IaaS) in future and, during the course of the project, Philips realised the IntelliSpace Discovery product, which targets academic hospitals worldwide to support the fast, solid development of new medical algorithms and prototypes that can be easily and quickly integrated in new products. By the end of 2020 Philips expects to support 140 applications annually for prototypes developed by academic hospitals.
Up and running
Three ITEA projects led by Frank van der Linden (Medolution and SoRTS) and Herman Stegehuis (BENEFIT) are still in progress. Philips will use the SoRTS innovations in embedded software to extend its range of interventional diagnostic imaging products. Within the project context, interventional MRI will take its first step from research tool towards a product for clinical practice thereby expand the MRI market. Van der Linden is confident that "most of the larger European hospitals will be installing one or multiple of image-based treatment delivery systems in the coming decade."
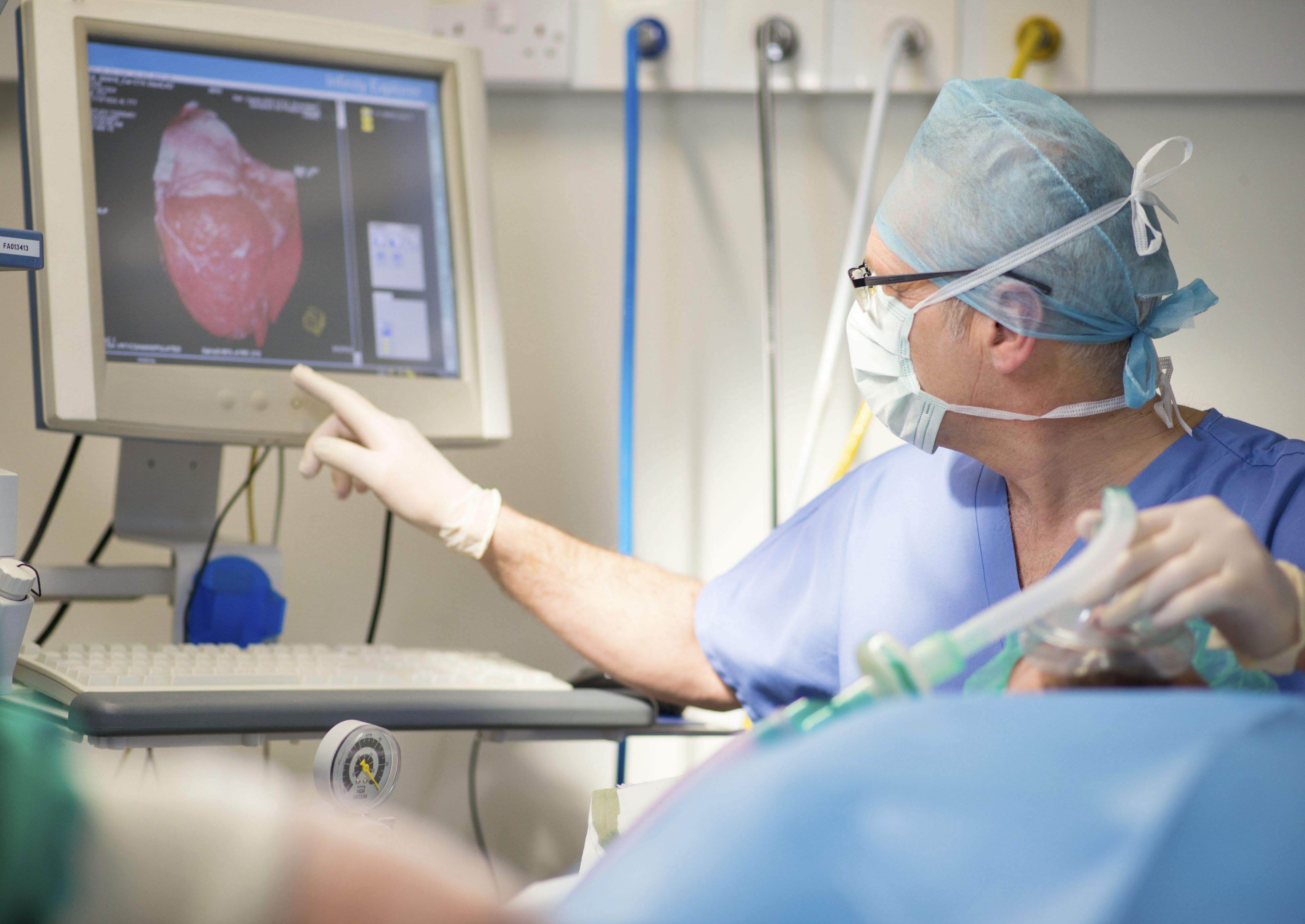
Herman Stegehuis is tasked with addressing three challenges in the BENEFIT project: societal (to cope with the increasing number of minimally invasive image guided interventions), economic (to deliver care with quantified targets in terms of quantity, price and quality of care) and technical (to show the technical feasibility of an integrated infrastructure that includes all relevant imaging and data sources, the modelling, analysis and presentation of these data and the integration into a Clinical Decision Support System).
BENEFIT brings together an industry-driven consortium of world-class complementary partners including universities and clinical end users to develop software analysis and imaging methods and tools that will present quantified information, personalised patient models and treatment alternatives before and during minimally invasive surgery procedures. "Ultimately," Stegehuis explains, "this fits in the trend of 'evidence based medicine' aiming to support physicians in decision making, to deliver care with quantified targets in terms of quantity, price and quality and to continuously measure, analyse and improve effectiveness and efficiency of targeted medical procedures."; As for Medolution, this project proposes reducing the cost of healthcare parallel with improving the patients' quality of life, creating smart environments that integrate professional and user created data. The tangible results will include early and pro-active decision support for patients and healthcare professionals through timely meaningful alerts and notifications, the ability to generate healthcare predictions based on continuous trend analysis and the sharing of healthcare data between devices and persons. By realising big healthcare data processing and analysis in the cloud, Medolution will deal with the challenge to integrate and combine enormous amounts of heterogeneous data and data sources, and extract relevant information yet ensure the safety and reliability of the devices in the patient's environment as well as the security and privacy of data.
"To quote Professor Oelfke from the Institute of Cancer Research in London: "In radiotherapy, we are trying to hit an invisible target with an invisible beam" … We don't want to estimate the tumour position, we want to see it during radiation delivery. MRI can offer this."
Professor Bas Raymakers, Department of Radiotherapy, University Medical Centre, Utrecht
On MRI (SoRTS)
Benefits all round
That healthcare is well and truly on the ITEA agenda is evident from an international customer workshop on Smart Health organised by ITEA in June to find out the concerns from the different stakeholders in the value chains about the desired functionalities or difficulties encountered in their daily environment. Casper Garos highlights the same need throughout the whole patient journey in developing strategic solutions for the continuum of care and underlines the commitment of Philips to ongoing research. Alluding to the words of the famous poet, T.S. Eliot*, he says that "we target tangible results in each project but the results at end of the project always signal a new beginning, prompt a new path in our ongoing drive to improve the lives and conditions of patients and clinicians alike, and ultimately the whole healthcare experience. The future is personalised medicine and that is certainly a key for our future direction."
* "What we call the beginning is often the end. And to make an end is to make a beginning. The end is where we start from." (from Four Quartets)
More information
Download Philips Healthcare Success storyRelated projects
BENEFITEdafmis
HiPiP
MEDIATE

